Redefining the “Epilepsy Journey” through Specialized Neuro-Rehab
In February 2026, International Epilepsy Day marked a pivotal shift in how we view neurological rehabilitation. The theme, “Milestones on My Epilepsy Journey,” emphasized that managing epilepsy is not merely about suppressing electrical surges in the brain—it is about reclaiming the physical autonomy that the condition often strips away.
For millions in India, particularly in the rapidly growing urban landscape of Bangalore and the underserved rural belts like Siddlaghatta, epilepsy is a diagnosis that carries a heavy weight of physical restriction. We are taught what a patient cannot do: “Don’t swim alone,” “Don’t climb ladders,” “Don’t exert yourself.”
At Rayara Kirana Physiotherapy, we are changing the narrative. We focus on what a patient can do. Through evidence-based neuro-physiotherapy, we are helping patients move from a state of “fragile protection” to “resilient movement.”
The Science of the “Seizure-Resilient” Body: Why You Need Physiotherapy for Epilepsy
To understand why physiotherapy is essential, we must look at how chronic seizures and long-term medication (ASMs) change the human body.
The Impact of Anti-Seizure Medications (ASMs) on Balance
While life-saving, many ASMs affect the cerebellum—the part of the brain responsible for balance and fine motor control. Patients often experience:
Ataxia: A lack of muscle coordination during voluntary movements.
Dizziness and Vertigo: Increasing the risk of falls even when a seizure isn’t occurring.
Bone Density Reduction: Certain medications interfere with Vitamin D metabolism, leading to a higher risk of fractures if a fall occurs.
Neuroplasticity and Movement
The brain is “plastic”—it can reorganize itself. Physiotherapy leverages Neuroplasticity. By engaging in repetitive, structured coordination exercises, we help the brain “hardwire” new pathways for balance and movement, providing a safety net for the patient when their primary neurological pathways are stressed.
The Multi-Faceted Benefits of Physiotherapy in Epilepsy Management
Pillar 1: Balance Training and Fall Prevention in Bangalore
A seizure can happen anywhere—in a kitchen, on a staircase, or walking through a crowded market in Bangalore. The primary goal of physiotherapy is to improve Proprioception (the body’s ability to sense its position).
Vestibular Rehabilitation: Exercises that stabilize the “internal leveling system” of the inner ear.
Core Strengthening: A strong core acts as a “shock absorber.” If a patient loses balance, a strong core allows for a faster “save” to prevent a hard fall.
Cardiovascular Health and Increasing the Seizure Threshold
There is a common myth that exercise triggers seizures. Scientifically, the opposite is often true. Aerobic exercise increases the “seizure threshold” for many patients. It stabilizes metabolic rates and reduces systemic inflammation. At Rayara Kirana, we monitor heart rate zones to ensure patients stay in a “Safe Zone” where they gain fitness without overtaxing the nervous system.
Post-Ictal Recovery Support and Muscle Rehabilitation
A “Grand Mal” or Tonic-Clonic seizure is the physical equivalent of running a marathon in three minutes. Every muscle in the body contracts violently, leading to:
Micro-tears in muscle fibers.
Joint displacement.
Severe lactic acid buildup.
Physiotherapy helps in the “washout” phase, using manual therapy and gentle stretching to speed up recovery and reduce the days spent in bed following an episode.
Pediatric Epilepsy: Supporting Growth and Developmental Milestones
For children, epilepsy is not just a medical condition; it is a developmental hurdle. Seizures occurring during critical “growth windows” can delay milestones like walking, jumping, or handwriting.
Neurodevelopmental Therapy (NDT) for Children
We use NDT to help children with epilepsy:
Cross-Lateral Movements: Helping the left and right sides of the brain communicate better.
Sensory Integration: Many children with epilepsy are hypersensitive to light or sound. Physiotherapy helps desensitize the nervous system to these triggers through controlled exposure.
Confidence in the Playground: We work on “safe falling” techniques, teaching children how to tuck and roll to protect their heads.
Addressing Stigma and Rural Healthcare Gaps in Siddlaghatta
The challenges in Bangalore Rural (Siddlaghatta) are vastly different from those in urban clinics. In rural India, epilepsy is often still viewed through the lens of “spirits” or “curses.”
The Rayara Kirana CSR Mission
Our outreach program in Siddlaghatta focuses on three key areas:
Caregiver Training: We teach families that holding a patient down during a seizure causes fractures. We teach “Safe Positioning” instead.
Home-Based Programs: Since many rural patients cannot travel to Bangalore daily, we design “No-Equipment” exercise routines that can be done in a small home setting.
School Integration: Educating local teachers that a child with epilepsy can participate in PT (Physical Training) class with basic precautions.
Safe Home Exercises for Epilepsy: A Guided Protocol
Disclaimer: Always consult your neurologist before starting a new routine.
| Exercise Category | Specific Movement | Purpose |
| Stability | Single-leg stand (with chair support) | Improves vestibular balance. |
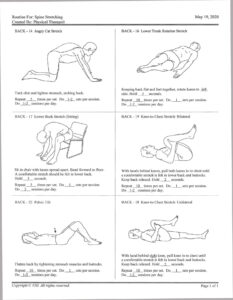
| Flexibility | Cat-Cow stretch | Relieves spinal tension post-seizure. |
| Respiratory | 4-7-8 Breathing | Lowers cortisol and stress levels. |
| Coordination | Balloon tapping | Enhances hand-eye tracking. |
| Endurance | “Laps” in a safe, carpeted room | Improves heart health without risk. |
Expert Commentary: Deep Insights into Neuro-Rehabilitation
Dr. Kiran, Senior Physiotherapist:
“In our Bangalore clinic, we see many young IT professionals with epilepsy. Their biggest trigger is ‘Photo-sensitivity’ and ‘Sleep Deprivation.’ We use physiotherapy to manage their circadian rhythms through evening relaxation protocols. We don’t just treat the body; we treat the lifestyle.”
Dr. Jain, Neuro-Rehab Specialist:
“When we talk about ‘Milestones,’ we mean the small victories. A patient being able to walk to the grocery store alone because they no longer fear a fall—that is the true power of integrated epilepsy care.”
Dr. Bhavana, Rehabilitation Consultant:
“Women with epilepsy face unique challenges, including hormonal triggers. Our physiotherapy programs are tailored to the female life cycle, ensuring safety during bone-density-critical years.”
Addressing Epilepsy Myths: Fact vs. Fiction
Myth: A patient should have a metal object in their hand during a seizure.
Fact: This is a dangerous myth in India. Placing metal (like keys) in the hand can cause injury to the patient or the caregiver. The best “support” is clear space and a soft pillow under the head.
Myth: People with epilepsy shouldn’t swim or play sports.
Fact: With a “Buddy System” and medical clearance, most sports are highly beneficial. In fact, many professional athletes manage epilepsy successfully.
Myth: Physiotherapy is only for people who are paralyzed.
Fact: Physiotherapy is for functional optimization. If your epilepsy makes you feel “clumsy” or “weak,” physiotherapy is the tool to fix it.
Lifestyle Strategies for Seizure Management: The “SEEP” Protocol
Movement is just one piece of the puzzle. At Rayara Kirana, we advocate for the “SEEP” protocol:
S – Sleep: Maintaining 7-9 hours to keep the brain’s electrical activity stable.
E – Eating: A low-glycemic diet helps maintain steady energy for the brain.
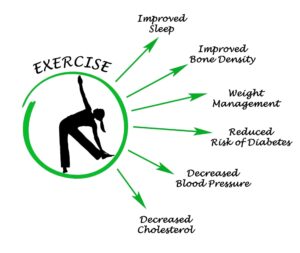
E – Exercise: 30 minutes of guided movement daily.
P – Prevention: Regular medical check-ups and physiotherapy assessments.
Epilepsy FAQ
1. Can physiotherapy help with the side effects of epilepsy medications?
Yes. Anti-seizure medications (ASMs) often cause side effects like dizziness, “fogginess,” and unsteadiness. Our neuro-physiotherapy protocols focus on vestibular (balance) training and core strengthening to counteract this “instability,” making you feel more grounded and alert.
2. What is the most important exercise for someone with epilepsy?
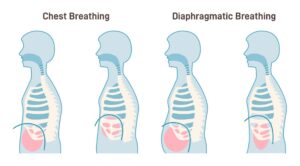
Stress is a major seizure trigger. Deep breathing switches the body from the “Fight or Flight” (Sympathetic) system to the “Rest and Digest” (Parasympathetic) system. This lowers cortisol levels and can help stabilize the brain’s electrical activity.
3. Is it safe to use heavy gym equipment?
We generally advise against heavy free weights (like barbells) unless you are under direct 1-on-1 supervision. Instead, we recommend resistance bands, cable machines, or fixed-track machines (like a seated leg press). These provide the same strength benefits without the risk of a heavy weight falling on you if a seizure occurs.
4. How do I know if I am over-exerting during a workout?
We teach the “Talk Test.” If you are too breathless to speak a full sentence while exercising, you are pushing too hard. Over-exhaustion can lower the seizure threshold, so it is important to slow down and let your heart rate recover.
5. Can physiotherapy help with the depression often linked to epilepsy?
Significantly. Epilepsy often leads to social withdrawal and “movement anxiety.” Exercise releases endorphins—the body’s natural “feel-good” chemicals. By rebuilding your physical confidence and independence, physiotherapy helps reduce the social anxiety and depression that often accompany the diagnosis.
6. Is it safe for me to walk or jog on Bangalore’s busy streets?
We recommend starting with treadmill training or walking in a controlled environment like a park (e.g., Cubbon Park) with a “buddy.” Once your balance and reaction times improve through physiotherapy, we can work on outdoor mobility strategies to keep you safe.
7. What is “Post-Ictal” physiotherapy?
This is therapy conducted after a major seizure. Seizures cause intense muscle contractions that lead to soreness and joint stiffness. We use gentle manual therapy, stretching, and myofascial release to help your muscles recover faster and reduce the physical “hangover” of a seizure.
8. Are there specific exercises that children with epilepsy should avoid?
Children should generally avoid activities with a high risk of head injury (like high-contact sports) without proper headgear. In our Siddlaghatta outreach, we teach children “Safe Falling” techniques—training the body to roll instinctively, which protects the head and neck.
9. Can physiotherapy help with “Aura” management?
While therapy doesn’t stop an aura (the warning sensation before a seizure), we train patients to recognize the physical signs. We teach “Safety Positioning”—the moment an aura is felt, the patient is trained to immediately sit or lie down in a specific position to prevent injury from a fall.
10. Does physiotherapy improve bone health in epilepsy patients?
Yes. Many long-term epilepsy medications can weaken the bones (osteoporosis). We incorporate Weight-Bearing Exercises (like walking or squats) and resistance training, which stimulates bone density and makes your skeletal system more resilient to fractures.
11. Can yoga be a part of my physiotherapy routine?
Yes, but with caution. While meditation and stretching are great, we advise avoiding Hot Yoga (overheating is a trigger) and Inversion Poses (like headstands) which can increase intracranial pressure. Always practice under the guidance of a neuro-specialist.
12. How often should I attend physiotherapy sessions?
For most patients, we recommend 2 sessions per week initially to learn safe techniques. Once you are confident and your balance scores improve, you can transition to a “Home-Based Maintenance Program” with monthly check-ins at our clinic.
13. Should my family members or caregivers attend the sessions?
We highly recommend it. At Rayara Kirana, we train caregivers in Seizure First-Aid. Knowing how to position a patient’s body during an episode is a physical skill that caregivers can learn right alongside the patient.
14. Are there rural support programs for those near Siddlaghatta?
Yes. Through our CSR initiative, we provide mobile screening camps and community-based rehabilitation. We believe that distance from Bangalore should not be a barrier to high-quality neurological care.
15. Can physiotherapy “cure” my epilepsy?
No. Physiotherapy is a supportive treatment. It works in tandem with the medication prescribed by your neurologist. While it doesn’t stop the electrical cause of epilepsy, it drastically improves your Quality of Life and reduces the physical complications associated with the condition.
Reclaiming Your Life through Quality Epilepsy Care
Epilepsy is a part of your life, but it does not have to be the entire story. As we embrace the advancements of 2026, we must look beyond the pill bottle.
The integration of physiotherapy into epilepsy care is more than just a medical trend; it is a movement toward dignity and independence. Whether you are navigating the busy streets of Bangalore or the quiet fields of Siddlaghatta, your physical health is your foundation.
Take the “Epilepsy Pledge” Today
If you or a family member has been living in the “shadow of restriction,” it is time to step into the light of rehabilitation. Our doors at Rayara Kirana Physiotherapy are open for consultations, screenings, and specialized neuro-rehab programs.
Contact us today to book your functional assessment.
Let’s move together, safely and confidently.


